When it comes to cardiovascular life support, one of the main steps is to find a solution for patients who can’t breathe for themselves. In the most basic form, a rescuer will breathe into the patient’s mouth and provide some oxygen through exhaled air. However, the rescuer must establish an airway as there has to be a direct connection between the flow of air and the patient’s lungs.

Oropharyngeal and nasopharyngeal airways are adjuncts that can be sued to obtain and maintain an open airway in a life support situation. One of the most critical decisions you will have to make when trying to save someone’s life is when to secure an advanced airway. It’s a crucial decision and must be quick, appropriate and effective. Here is what you need to know about these two interventions and their pros and cons.
Oropharyngeal vs Nasopharyngeal Airways
The decision to intubate is the first step in the placement of an advanced airway. It should be based on your primary survey, including the patient’s O2 saturation and vital signs as well. When a patient is in respiratory distress, he or she will present signs and symptoms such as the following.
- Mild anxiety
- Normal LOC
- Tachycardia
- Chest tightness
- Decreased O2 saturation
- Altered breath sounds
- Cyanosis (if present, should be minimal)
While these signs may not be serious enough to warrant an oropharyngeal or nasopharyngeal airway, a patient who is approaching failure will present the following symptoms, which indicate the need for immediate airway intervention.

- Altered mental status, and if it’s less than 8, you need to intubate immediately
- Tachycardia, more than 130 bpm
- Use of accessory muscles/retraction
- Absent breath sounds
- Abnormal respiratory patterns
- Decreased O2 saturation
- Diaphoresis and pale skin
- Cyanosis
Intubation has several advantages for controlling the airway. For oral intubation, you can opt for oropharyngeal airway, while for nasal intubation, you can choose nasopharyngeal airway. Following your patient assessment, you can determine if oral or nasal intubation will be the best choice for controlling the airway.
What is an Oropharyngeal Airway Used for?
As the name implies, an oropharyngeal airway (OPA) is placed in the patient’s mouth and the distal end should stop at the level of the pharynx. It’s also known as an oral airway, a Guedel pattern airway or Guedel airway, named after the original designer Arthur Guedel.
It’s safe to use this airway in a deeply unresponsive patient, unconscious patient or an anesthetised patient because the gag reflex is depressed and will prevent gagging and vomiting of gastric contents. Oropharyngeal airways come in different sizes and you need to make sure to pick the right size for your patient.
The easiest way to get a rough sense of the size needed is by placing the airway at the side of the patient’s face and seeing whether it will extend into the pharynx. If the distal part of the airway reaches the mandible and the flange is at the patient’s lips, then you have the right size. When placing the OPA, it’s important to not press the tongue into the airway.
Before inserting the OPA, clear the patient’s mouth of secretions such as blood, vomit or sputum using a suction catheter. Then place the OPA in the mouth with the curved end towards the hard palate or the roof of the mouth. You can turn the curve of the device 90 or 180 respective to its final position before inserting it. Once the airway is advanced into the pharynx, then the device can be rotated into place.
What is a Nasopharyngeal Airway Used for?
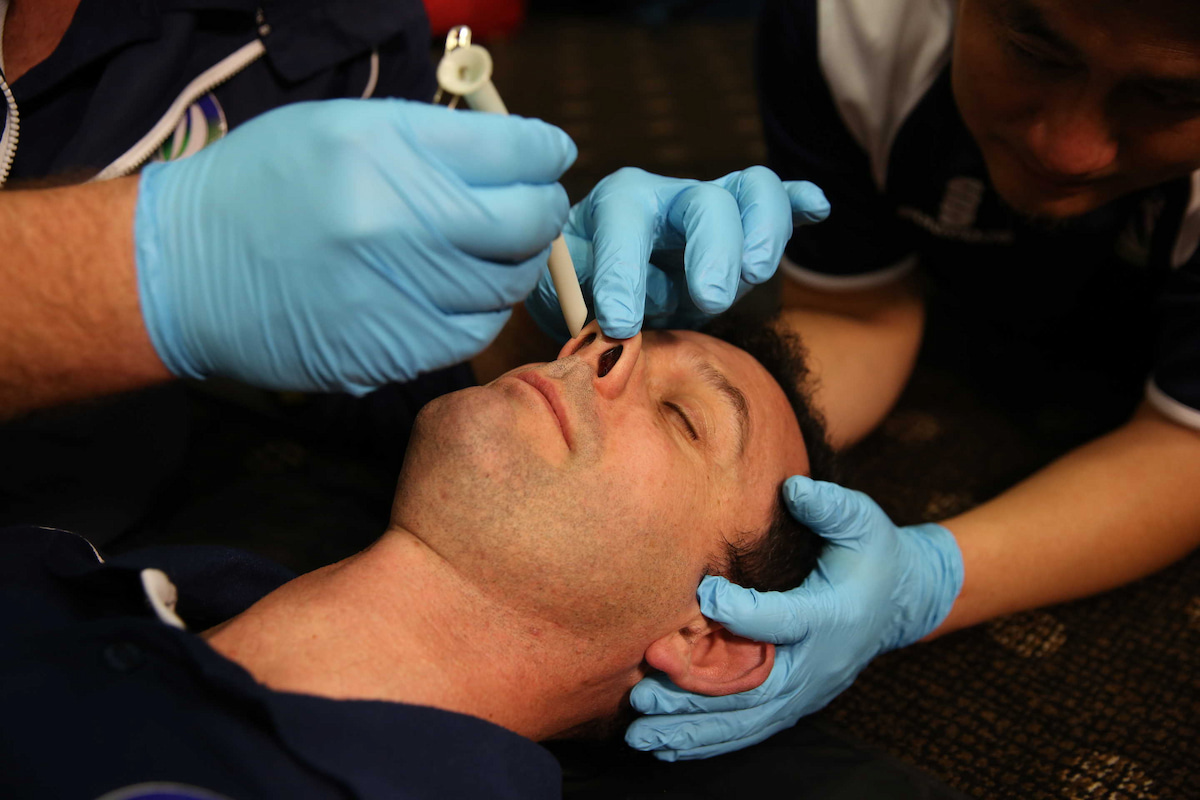
A nasopharyngeal airway (NPA) is inserted through the patient’s nose and the distal end stops at the level of the pharynx. It’s also referred to as a nasal airway, NPAT or nasopharyngeal airway tube or nasal trumpet.
This type of airway has some advantages over the OPA as it can be used in a conscious, unconscious or semi-conscious patient since it doesn’t stimulate the gag reflex as an OPA does. Also, an NPA can be used in patients with mouth trauma, where an OPA can’t or shouldn’t be used.
Same as oropharyngeal airways, nasopharyngeal airways come in different sizes and to get a rough sense of the right size, you can follow the same approach as mentioned above. Place the airway at the side of the patient’s face and align it with the nose instead of the mouth. To determine the right size, measure from the tip of the patient’s nose to the tip of their earlobe. Always choose an NPA that has a diameter a little smaller than the patient’s nares.

When inserting an NPA, it’s important to remember that the nostrils extend posteriorly, not caudally, meaning that the tube should be placed towards the back of the head and not towards the top of the head. Make sure to lubricate the NPA before inserting it with a water-based lubricant to facilitate a less traumatic insertion. Once the NPA is inserted, the flange should rest on the nostril opening.
Contraindications
Using advanced airways has a lot of advantages, however, there are some contraindications you should be aware of. Using an OPA on a conscious patient with an intact gag reflex is contraindicated. A patient that can cough still has a gag reflex and using an OPA is not recommended. Also, if the patient has a foreign body obstructing the airway, avoid using an OPA.
An NPA, on the other hand, should not be used on a patient who has an actively bleeding nose or nasal fracture. Sometimes slight bleeding may occur when you insert the NPA and it should be wiped away or suctioned right away.